In late 2023, running from my house to the garage, I caught the very front edge of a stair. As my heel sank down, my body kept moving forward, and I felt a tremendous buildup of pressure in my calf, then a firm “pop.” No more pressure. I knew what happened immediately. I hopped to the house on one leg, pulled my boot off and could see my heel and calf weren’t connected by my achilles tendon anymore. As a physical therapist, I knew this was bad–I’d helped lots of patients after tearing their own achilles. I was freaked out about what this would mean for me, because I walked every day, ran most, went to the gym regularly, and I had a professional dance show coming up in 4 months.
I’ll tell you what I learned from my experience as a physical therapist turned patient–my timeline, my mistakes, and my approach to recovering from an achilles surgery; a surgery with a notoriously long rehab timeline. And if you’re concerned you are not on track, I work with people one-on-one in my virtual PT clinic to make sure their recovery is going how it’s supposed to. You can schedule a free consult, here.
The First Two Weeks After Surgery Sucked
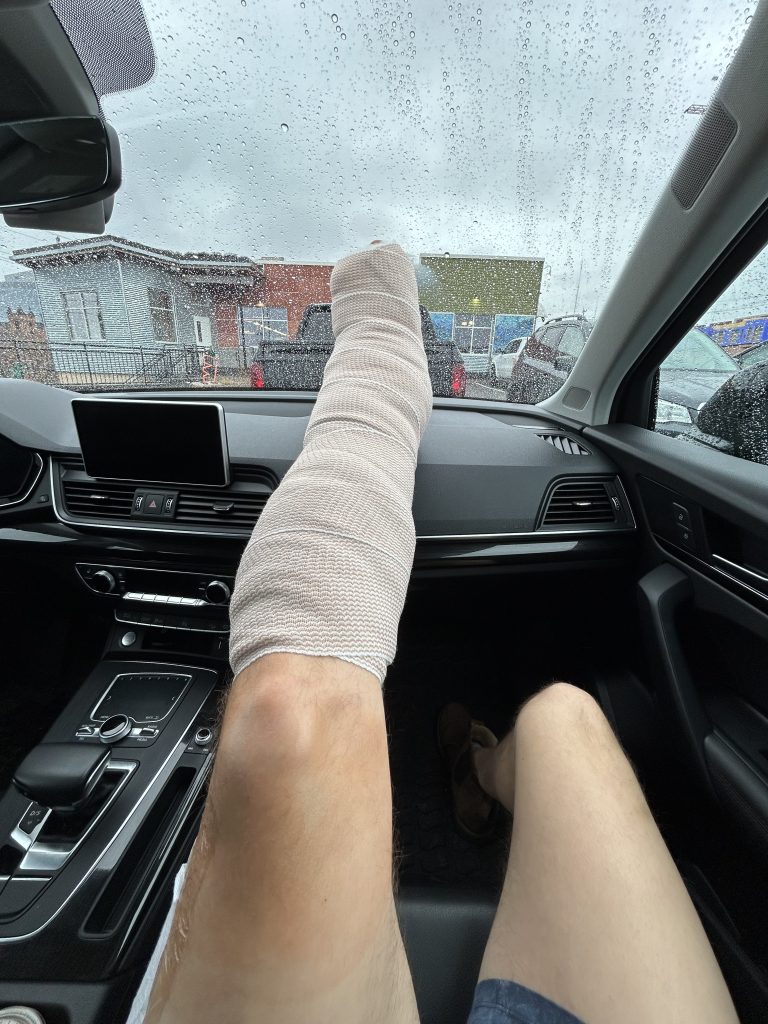
With my foot trapped in a splint, the first two weeks after surgery were hard. Three weeks of strict nonweight bearing are normal, which means you’re either on crutches, a knee scooter, or a walker depending on your coordination and home setup. I even tried one of those weird knee crutches that makes you look like a pirate, but I found it way too cumbersome. I went with crutches, because our house had a lot of stairs, and knee scooters are a pain to lug up and down. But crutches occupy your hands, so I couldn’t carry anything from the kitchen to the living room, and I felt a little helpless army crawling my dinner plate across the living room floor.
Then there was the pain. It hurt the worst at night trying to sleep, because the back of my calf pressed against the splint and made everything really achy and crampy. Waking up for bathroom trips was an adventure fumbling with crutches in the dark and trying not to step onto my foot.
The first couple weeks in the splint, the only rehab-specific exercise I worked on was isometric contractions of my calf. I would very very lightly press the ball of my foot into the splint and hold for 3 seconds. I was trying to encourage regrowth between the two frayed ends of my achilles that had been sewn together, but I didn’t want to create too much force too soon. Otherwise, I kept up at the gym focusing on upper body, and I started using the arm bike I’d never used that sat near the stationary bikes.
Returning to Weight Bearing After Achilles Surgery
Mass General has a good rehab timeline following surgery, which recommends 3 weeks without any weight through your foot. I returned to weight bearing 2 weeks after surgery, which was too soon, and my body knew it. The physician assistant I saw after surgery transitioned me to a walking boot and told me I could be “weight bearing as tolerated.” For me, it took another couple weeks before my foot would tolerate the weight of my body. Here is a video on tips for fitting your walking boot, if you’re curious.
I was lucky to have medical and rehab knowledge when I was transitioned to a walking boot. I knew how to work my way into full weight bearing, and how to slowly move from using two crutches to using one crutch. Most people do not know how to make these types of transitions, and I have seen many patients over the years go too quickly from using a cane, or a crutch, or a boot, to walking with nothing at all. These patients develop major limps, lots of other compensations, and they usually hurt. When I ask them why they aren’t using their boot or walker, they say “the doctor told me I didn’t need to anymore.” But based on how they were moving, their bodies still clearly wanted the extra support.
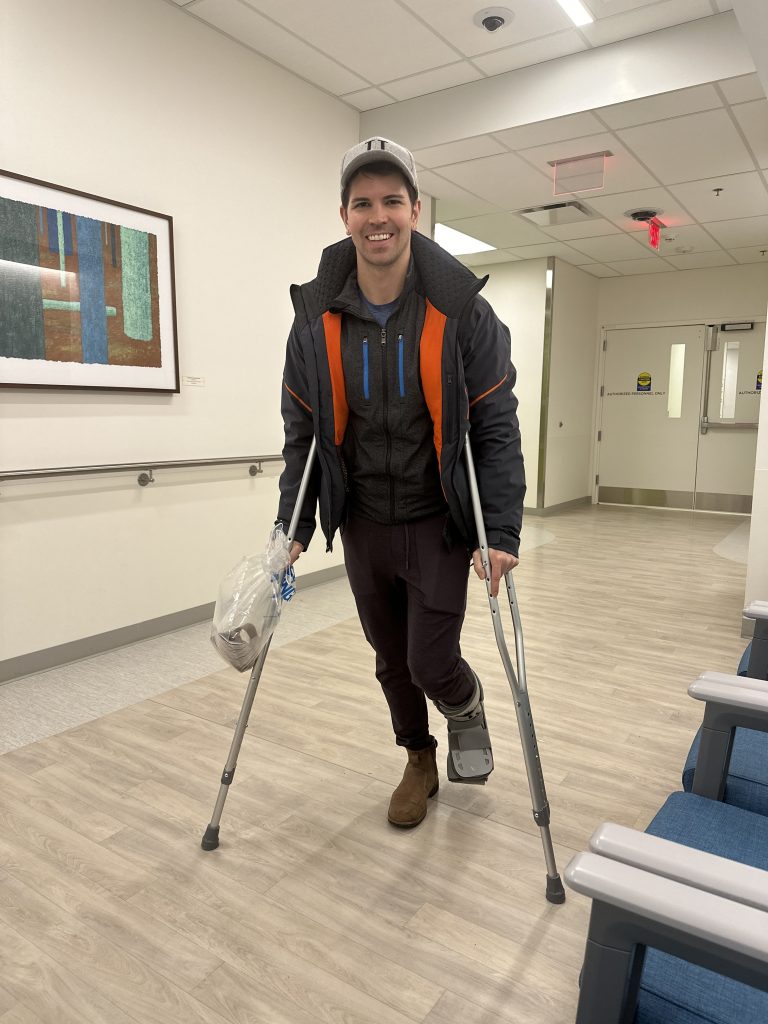
So take this as a lesson: moving from one weight bearing status to another is a process. Weaning from a device like crutches or a boot is a process. If you gradually work your way through this process, you’ll be much better off than making an abrupt transition that your body isn’t ready for.
The Rehab Focus After Getting Out of A Splint
After my splint was off, weeks 3-6 were spent working on active range of motion at my ankle. It was hard work to get my ankle to point, and I kept up with my isometric contractions, asking for a little bit more contraction of my calf each week. I couldn’t put full weight through my foot and kept using the crutches, gradually adding more weight to my leg week to week until I could walk without a big limp or major pain by week 7 or 8.
I DID NOT stretch my calf, and you shouldn’t either. I had been warned about and read into the risks of stretching your calf in this phase of recovery. Overstretching can create a long, weak tendon that won’t support you long term and increases the risk of a failed surgery. So I did not stretch it past neutral (trying to get your ankle to a 90 degree angle). Standing still on both legs achieves this, as a reference.
To ensure your tendon doesn’t get overstretched, it’s common practice to have wedges inside the walking boot that lift up the heel. The wedges put your foot at an angle that’s much nicer for your calf and achilles at this stage, and the idea is to slowly reduce the amount of wedging you use over the course of several weeks. It’s a lot to consider and manage, which is why I recommend everyone work with a physical therapist throughout your recovery after surgery. I don’t care if someone told you that you don’t need to do PT, because PT is going to help your recovery go smoother, and there’s a lot you don’t know about the recovery process. You don’t have to go into a clinic, and you can work online with someone like me, but you need a guide to make sure you’re on track and help you advance to the next stages. Okay, I’ll get off that soapbox now.
Working From the Boot to Shoes

It took me two full months to start transitioning away from the walking boot and using shoes in the house, which is the expected timeline. Remember, you’re dealing with a tendon repairing from a major surgery. This isn’t about when you’re ready to advance, it’s about when your tendon is ready to advance. You can’t rush it.
I’d slowly gotten rid of the wedges in my boot to increase the stretch on my ankle, but I added a heel lift to my shoe for around the house. A boot locks your ankle into a specific degree of bend, but walking in a shoe creates more freedom and requires a lot more ankle flexibility. Heel lifts help because walking can put a big stretch on your calf and achilles, and taking a step with a heel lift means you can take a longer step without putting as much stretch on your recovering tendon.
At two months, I started training heel raises using both feet but shifting a good amount of weight away from my healing ankle. Over the course of weeks I started being able to heel raise with even weight, and I slowly advanced to eccentric heel raises, where I put more weight through the surgical side as I lowered down.
At two months, I also started training my single leg balance, which was terrible. I was a dancer who had a show in 6 weeks, and I couldn’t balance more than 3 seconds on one leg. Great. I would probably advise most patients away from trying what I was trying, but I was bull-headed that I was going to participate in this dance show; I just didn’t know how yet.
Going From Walking to Dancing
At three months, my calf was puny compared to the other leg; it looked like I had one mommy calf and one baby calf. Still, I was less concerned about the appearance and more concerned that, at three months, my legs were functioning at significantly different levels. This is normal, and, for most people, different aspects of recovery will take over a year. But I didn’t have a year, so I started wearing shoes with heel lifts around town, and I gradually worked my way off of my walking boot for the longer mile or so walks I was taking to and from the gym. But walking was slow, and it felt heavy. I couldn’t push off the toes of my back foot, because that required too much force through my achilles tendon. By the end of most walks, or most days, I was sore.
Rehearsals for the show started, and I was not dancing even close to the same way I used to. I could not dance in flat shoes because it required ankle flexibility I didn’t have and wasn’t ready for, so I had to come up with a creative solution.
Instead of wearing dance shoes, I bought black combat boots with a 3” heel, and they worked amazingly. They lifted my heels up high enough that I could bend my knees and take longer steps without hurting, and they even fit with the style of the show.
I could not jump. And if you’re recovering from an achilles surgery, it’s very unlikely you’ll be jumping at 4 months into recovery. It won’t be for lack of wanting to or trying hard enough, it’s because your achilles isn’t ready.
The Show and the Rest of My Recovery
The show came, and I was able to get through it. I had to modify, I had to use my boots with the heel, and it wasn’t pain-free, but I did it. As a physical therapist, I try honoring my clients’ goals, even when I don’t love them. I’ve had dancers who want to compete with sprained ankles, skiers who are going on big trips with meniscus tears, and patients with shoulder injuries who want to get back to pickleball. The easy answer in all these situations would be to say “just don’t do it.” We could take things slow, and let them be active again if and when they feel all better. But that’s not the right answer.

Our activities and hobbies and interests are what makes life interesting. These are the things that fuel us and give us satisfaction. They matter. And when medical providers tell people “don’t dance,” or “don’t run,” or “don’t do that thing you love anymore,” I think it’s a disservice. Things that make us happy are worth doing, and there are 100 ways to modify or work into something safely so you can keep doing them.
Achilles recovery is a long road. It was 6 months before I could do any kind of running, almost a year before I could walk for miles without noticing it, and a couple years later I’m still working on my single leg calf strength and flexibility. But I can do the things I want and love, and so can you.
What Should I Do Next?
If you want to get your recovery started and make sure you’re doing the right exercises to get you feeling better, you can work with me. I do everything online with my studio, motivPT. And studies show that patients are more likely to stick with their exercises when received through telehealth. Which is good news for everyone, because people who do their home exercises hurt less, function better and have improved quality of life in the short term and maintain those things in the long term.
I, Dr. Alex, am here to support you every step of the way, no matter where you are. Book your free 15-minute consult to talk with me about your concerns and learn more about how we work! My online physical therapy and personal training can help you regain what you thought you’d lost and go strongly into your future.
At motivPT, we believe your body deserves to feel great.